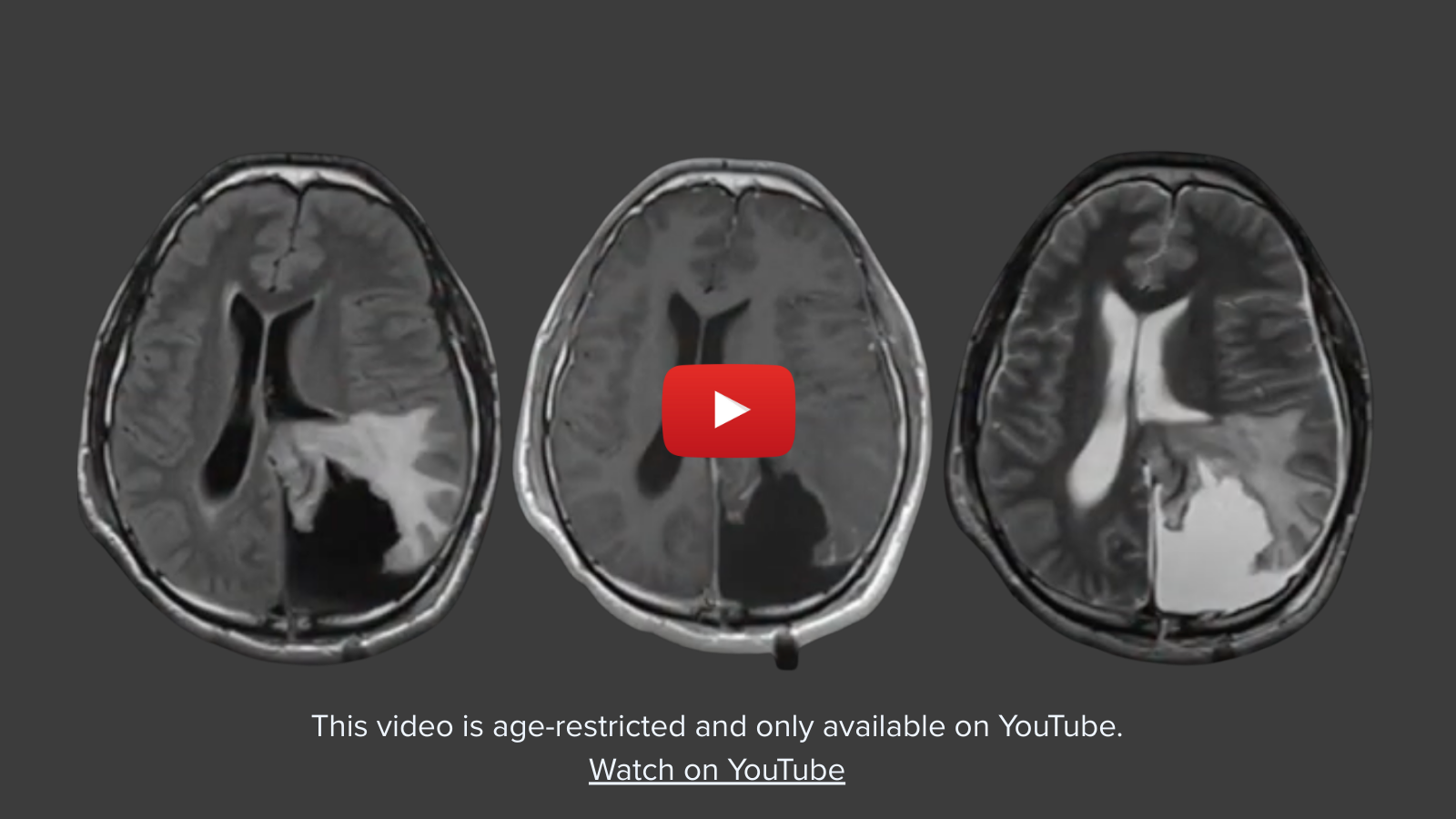
New Jersey Brain & Spine’s expert team of neurosurgeons is trained in the most advanced and cutting-edge techniques including fluorescence-guided tumor resection. This is just one of the innovative treatments we offer to help provide the highest quality and most minimally invasive approaches to brain tumor removal.
What is fluorescence-guided—or fluorescent-guided—tumor resection?
Fluorescence-guided tumor resection is a new technique that offers greater precision by helping surgeons visualize and distinguish between cancerous and healthy tissues while they are operating.
Non-toxic fluorescent agents such as 5-aminolevulinic acid (5-ALA) and indocyanine green (ICG), illuminate brain or spinal tumors, cancerous cells, nerves, and features, creating a glowing map of sorts that guides surgeons during operations.
How does fluorescence-guided surgery work?
A fluorescent agent is administered preoperatively. Tumor cells absorb the agent, and during surgery, specialized cameras and lighting make the tumor “glow.” Surgeons use this fluorescence to distinguish between cancerous and non-cancerous tissue for more precise resection.
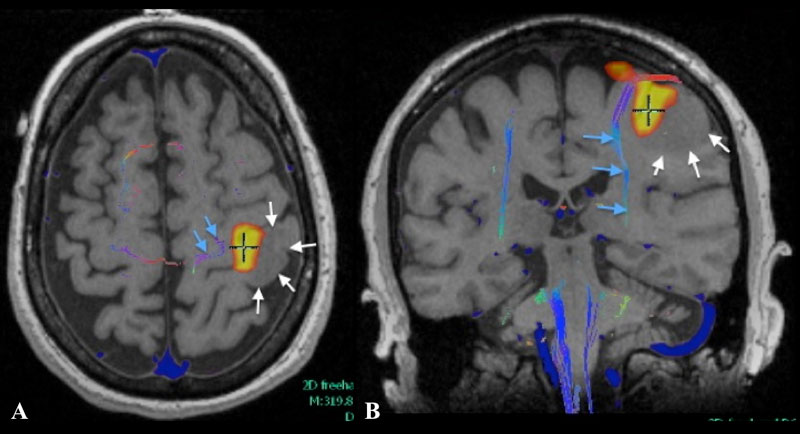
Axial (A) and coronal (B) T1 weighted MR fMRI localizing hand function with relation more laterally placed hypo-intense neoplastic process (white arrows) with more medially situated descending motor fibers of cortico-spinal tract as indicated by MR tractography.
Intraoperative images taken at surgery with normal light (top left) showing no evident tumor. Intraoperative image of the same field with Yellow 560 filter (bottom left) showing area of fluorescence (F) and non-fluorescent area (NF). Right upper H&E stain showing normal brain obtained from NF area whereas F area diagnostic for high-grade glioma.
What is the surgical benefit of utilizing 5-ALA for fluorescence-guided surgery of malignant gliomas?
There are several benefits to leveraging fluorescent agents to help guide resection of brain tumors, including malignant gliomas:
- The glowing cells allow for better visualization of tumor margins, helping to ensure the surgeon leaves no cancerous cells behind.
- By helping to reduce the risk of leaving behind residual tumor tissue, the likelihood of occurrence of future tumor spread is reduced, improving overall long-term outcomes.
- The agents help specifically target cancerous cells, ensuring that healthy tissues and brain structures are left undisturbed. This reduces the risk of surgical complication within delicate brain structures and areas of dense tissue or low visibility.
- The increased visibility helps improve intraoperative decision-making, decreasing the likelihood of needing follow-up surgeries and improving both quality of life and recovery time.
What are the limitations?
There are several limitations surrounding fluorescence-guided surgery:
- Dependence on fluorescent uptake: Some tumors may not absorb the agent uniformly, leading to incomplete visualization.
- Tissue penetration: Fluorescence may not penetrate deeply enough for larger or deep-seated tumors.
- False positives/negatives: Occasionally, non-tumor tissues may fluoresce, or tumor tissues may not absorb the agent as expected, leading to misidentification.
What is recovery like?
Recovery from fluorescence-guided tumor resection is similar to other types of brain surgery; however, the heightened level of precision may help reduce complications and eliminate the need for future or additional invasive open-brain surgeries.
Case Study: Successful Treatment of a Patient with fluorescence-guided tumor resection
Dave, 52-year-old data scientist, began experiencing headaches, had a foggy memory, and left-sided weakness. Magnetic resonance imaging (MRI) revealed a high-grade glioma, which was confirmed via biopsy. The tumor was located near eloquent brain areas, which when damaged, can lead to neurological challenges, including speech problems, paralysis, or loss of sensory perception.
The team at New Jersey Brain & Spine opted for fluorescence-guided resection using 5-aminolevulinic acid (5-ALA) to enhance tumor visualization under specific lighting, allowing for more complete tumor removal while preserving Dave’s healthy brain tissue. Four hours prior to surgery, Dave ingested 5-ALA orally. During the operation, the tumor fluoresced under blue light, allowing the surgeon to differentiate malignant cells from normal brain tissue with greater precision. The surgery was completed without neurological complications, and recovery was uneventful.
Dave was discharged five days after his operation and returned to light daily activities within two weeks. Follow-up assessments over six months showed improved cognitive performance and motor function. The clinicians at New Jersey Brain & Spine will continue to monitor Dave’s progress, but note that a more thorough removal of cancerous tissue via fluorescence-guided tumor resection typically reduces recurrence rates.
Compassionate, Expert Care at New Jersey Brain and Spine
The team at New Jersey Brain & Spine is one of the leading practices in the Tri-State region offering fluorescence-guided resection for multiple conditions.
If you have questions about the benefits, or would like to discuss your specific situation, please don’t hesitate to reach out to New Jersey Brain and Spine. Our surgeons are among the most experienced in the region — and top-ranked nationally — and are committed to delivering personalized, patient-centered care that prioritizes health, function, and quality of life. Contact us today to schedule a consultation.